
Testing and Diagnosis
It can be difficult to determine through testing, if someone has Mast Cell Activation Syndrome (MCAS). There isn't a definitive test and many of the symptoms overlap with other conditions. Also, each person presents with different symptoms. This is why the diagnostic criteria combines testing with clinical observation.

Why Testing for MCAS Is Complex
Mast cells release chemicals called “mediators” when they’re active. However these chemicals (such as histamine, tryptase and others) don’t stay high all the time, and many break down quickly in the body. Levels often rise during a symptom flare and then return to baseline relatively fast.
This means:
- A test taken when you are not experiencing symptoms may come back within the normal range, even if MCAS is present.
- A test taken during a symptomatic episode may still be normal if the mediator has already peaked and fallen, or if the specific mediator being measured is not the one driving that flare.
- No single laboratory test can definitively confirm or exclude MCAS on its own.
For this reason, testing is usually interpreted alongside the wider clinical picture. This may include your pattern of symptoms over time, evidence of mast cell mediator involvement, response to treatment, and careful assessment to rule out other possible conditions.
Diagnosis is therefore often based on a combination of clinical history, laboratory findings (where present), and professional judgement, rather than one standalone test result.
What Does Diagnosis Involve?
Diagnosing MCAS can take time. For many people, the process involves careful assessment over months or even years.
Recognising Symptoms: Doctors look at your symptoms over time. MCAS doesn’t just show up in one part of the body, it always involves multiple body systems and can involve skin, gut, breathing, heart rate, brain fog, and more. Symptoms can come and go, and their severity can change over time, which makes it harder to pin down. You can use our symptom tracker to help keep a record.
Response to Treatment: Sometimes, doctors may try medications commonly used for MCAS (like antihistamines or mast cell stabilisers) to see whether your symptoms improve. A positive response can be a clue that mast cells are involved. This is sometimes called a treatment trial.
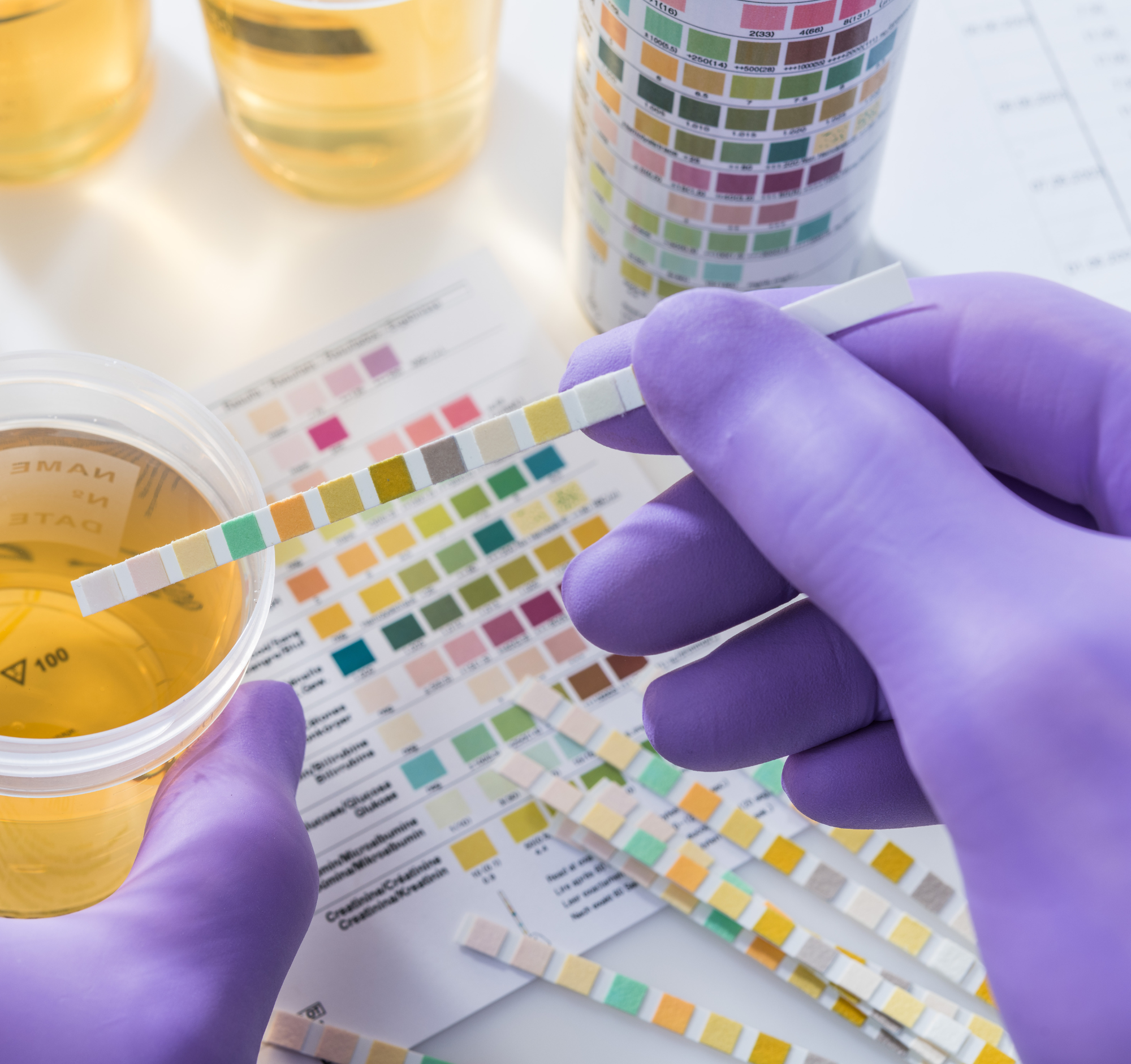
Mediator Testing (Blood & Urine Tests): Mediator tests look for chemicals released by mast cells, such as histamine or prostaglandins, which can go up during flares. These tests are most useful when done during a flare rather than when symptoms are calm, because mast cell products quickly return to normal levels. There’s no single test that can confirm MCAS by itself. A normal result doesn’t definitely rule it out, and a raised result doesn’t always mean MCAS on its own, which is why tests are only one piece of the diagnostic process.
Ruling Out Other Conditions: Because MCAS symptoms often overlaps with many other conditions (like EDS, PoTS, autoimmune diseases and more), doctors will often look at other possible causes before or alongside testing. This can help make sure nothing else is being missed and you get the best care for your personal circumstances.

Types of Tests People May Have
If your clinician suspects MCAS, you may be offered the following tests:
Blood Test: Serum Tryptase
In Mast Cell Activation Syndrome, baseline tryptase is often normal and many people do not show a significant rise during flares. High tryptase is more likely associated with other conditions like systemic mastocytosis or anaphylaxis.
It is important to acknowledge that many clinicians view tryptase as an essential marker because it is currently the most standardised and widely studied mediator available. From a medical perspective, objective evidence matters - and tryptase remains the most established test within formal diagnostic frameworks.
This can sometimes create tension in practice. Those affected may have clear, multi-system symptoms but normal tryptase results. Awareness in this area is evolving. Research is ongoing into additional mediators and improved testing methods.
At Mast Cell Action, we are working to improve professional education, encourage research into better biomarkers, support clearer clinical pathways and promote understanding of the limitations of current testing.
If you have normal tryptase but ongoing symptoms, it is reasonable to discuss this with your healthcare professional within the context of the full diagnostic picture.
Urine Tests: Mediators Over 24 Hours
These look for breakdown products of chemicals which are released by mast cells. Key mediators include:
- N-methylhistamine, which is a histamine marker that can show mast cell activity.
- Prostaglandins, which can reflect mast cell activity, though they may also come from other cells.
Because mast cell chemicals vary throughout the day and with flares, a 24-hour urine collection is usually recommended to give a fuller picture.

What Test Results Mean
- Elevated mediator levels can suggest mast cell activity and can support a diagnosis.
- Normal results do not rule out MCAS, especially if symptoms don’t happen during the test period.
- Test results are most powerful when combined with your symptom history and clinical findings.
That’s why many people will go through a mix of symptom tracking, treatment trials, and testing before a healthcare provider feels confident making a diagnosis.
Diagnosis isn’t usually quick as symptoms vary widely between people, tests are not widely available and not always reliable, and doctors may not be familiar with them. It is often possible to gain some relief from symptoms by focusing on treating the most troublesome symptoms even without diagnosis.
You may be diagnosed as “suspected MCAS” if all the pieces aren’t yet clear.

Talk to Your GP
If you think your symptoms may be related to mast cell activation, your GP is usually the first step in the process. We know that starting this conversation can feel daunting, especially if your symptoms are fluctuating, complex, or have previously been dismissed. Being prepared can help you feel more confident and ensure the appointment is as productive as possible.
It can be helpful to keep a simple symptom diary, noting how often symptoms occur and whether they happen in flares and recording any known triggers. You might also find it helpful to list any medications or treatments that have helped and bring copies of any relevant test results. Patterns matter in MCAS. Clear, organised information can support your GP in seeing the bigger picture.
Your GP may want to rule out more common conditions first. This is a normal and important part of safe medical practice.
Resources like our MCAS Testing leaflet, can be helpful - especially if your GP isn't familiar with MCAS.
You don’t have to navigate this alone. We have resources and community support to help you prepare for appointments and make your story heard.

About Referrals
There is currently no single “MCAS clinic” pathway in the UK. Referral may be to allergy or immunology, haematology, gastroenterology, cardiology, or another relevant specialty depending on your symptoms.
In some areas, awareness of MCAS is still developing. This can mean experiences vary. If you feel unsure about next steps, it is reasonable to ask:
- What conditions are being considered?
- What tests are planned and why?
- What would happen if results are normal but symptoms continue?

If You Feel Dismissed
Sadly, some people report feeling unheard during their diagnostic journey.
If this happens, you may find it helpful to stay calm and focused on your symptoms, ask for clarification of the clinical reasoning and consider requesting a second opinion.
Bringing written information and resources can also be useful.
It can take time to reach clarity with complex, multi-system conditions.
At Mast Cell Action, we believe that everyone deserves informed, respectful care. Our goal is to support you with clear information so you can have constructive conversations with your healthcare team.

Support Along the Way
Because MCAS doesn’t yet have widespread agreed standards in the NHS, experiences can vary. Some people are able to access specialist testing and support; others may find it hard to get tests arranged.
We know that pursuing testing and diagnosis can be stressful, especially when results are normal or unclear. This can feel frustrating, but you’re not alone, and there are ways to work with your GP to find the right pathway for you.
You don’t have to navigate it alone. Mast Cell Action has resources, leaflets you can share with clinicians, and support services that can help you understand your journey and plan your next steps.
Become a friend
Sign up to become a Friend of Mast Cell Action so we can keep you up to date on our progress and on how to get involved in our latest campaigns and initiatives.
Donate
Mast Cell Action relies entirely on the generosity of people like you. Please make a donation now and together we can make a difference to those affected by MCAS.







